Bedsore Life Expectancy: What You Should Know (Infographic)
Call: (312) 609-0400
or fill out the Contact Form

What Is Bedsore Life Expectancy?
Bedsore life expectancy depends on the stage of the pressure sore, the resident’s overall health, how quickly treatment begins, and whether complications such as sepsis, cellulitis, bone infection, or organ failure develop. Stage 1 and Stage 2 bedsores may heal with prompt care, but Stage 3 and Stage 4 bedsores can become life-threatening, especially for elderly nursing home residents.
Bedsores are a common warning sign of nursing home neglect, and family members should take quick action once their presence is discovered. They occur when there is unrelieved pressure on the skin and can lead to serious, potentially life-threatening infections.
(Article continues below infographic)
The Prevalence of Bedsores
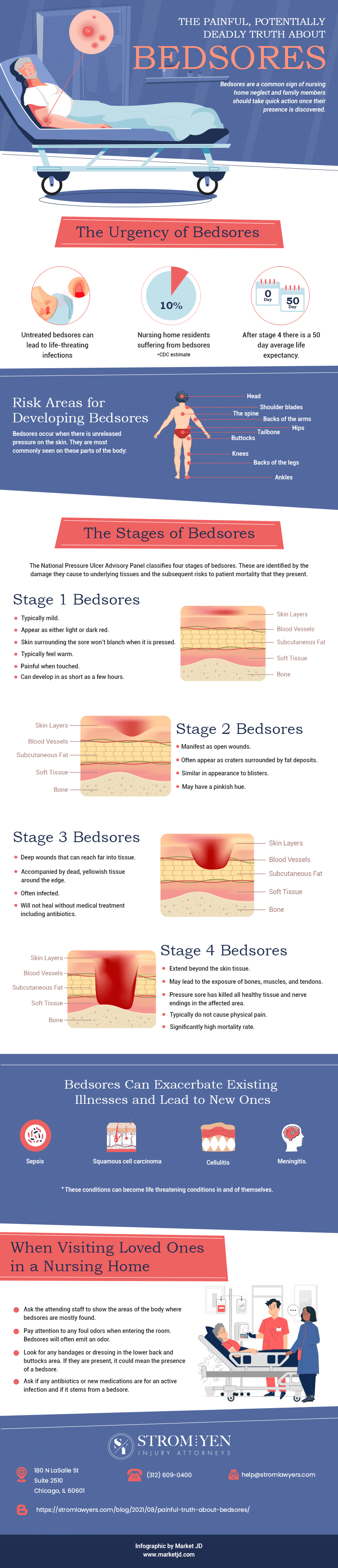
The CDC estimates that as many as 10% of nursing home residents suffer from bedsores. It is far from a new problem, and the prevalence of bedsores in nursing homes has been recognized for decades. Studies conducted by the National Pressure Ulcer Advisory Panel, CDC, and other entities have drawn a direct correlation between the presence of bedsores and patient mortality. The more advanced the bedsore, the greater the possibility that the nursing home resident will pass away from the injury. By some accounts, patients with Stage 4 bedsores have an average life expectancy of just 50 days once the condition has progressed to that level of severity.
Risk Factors for Developing Bedsores
While every nursing home resident is at risk for developing bedsores, some residents face greater risk than others. Individuals who depend on wheelchairs or are confined to bed for long periods of time are especially vulnerable. Pressure sores can be caused by friction between the skin and clothing or bedding, shearing when skin tissue is pulled in the opposite direction from bone structures, or sustained pressure when a nursing home resident's body is immobile for an extended period of time. When staff fail to monitor and reposition vulnerable residents, families may need to speak with an Illinois nursing home neglect lawyer.
Bedsores can be found on all areas of the body. However, they are most commonly seen on the buttocks, tailbone, backs of the arms and legs, the spine, shoulder blades, head, knees, ankles, and hips. This is because these areas are typically those that the weight of an individual's body will rest upon while laying or sitting.
Bedsore Stages
The NPUAP classifies four bedsore stages. These are identified by the damage they cause to underlying tissues and the risks they may present to patient health and mortality. Bedsores can develop quickly and may progress at different rates depending on the patient's overall health and whether prompt bedsore treatment is provided. If a nursing home allows a pressure sore to worsen without appropriate care, the resident’s family may have grounds to investigate a nursing home neglect claim.
| Bedsore Stage | What It Means | Life Expectancy / Health Risk |
|---|---|---|
| Stage 1 | The skin is red or discolored and may feel warm, painful, firm, or soft. The skin has not yet opened. | Stage 1 bedsores are usually treatable when they are identified early and pressure is relieved quickly. |
| Stage 2 | The sore becomes an open wound or blister-like injury affecting the outer layers of skin. | Stage 2 bedsores may heal with proper wound care, but the risk of infection increases if treatment is delayed. |
| Stage 3 | The wound extends deeper into the tissue below the skin and may show dead tissue, drainage, or signs of infection. | Stage 3 bedsores are serious injuries that can lead to long-term complications, infection, hospitalization, or worsening health. |
| Stage 4 | The wound extends through the skin and tissue and may expose muscle, tendon, or bone. | Stage 4 bedsores can become life-threatening, especially if the resident develops sepsis, bone infection, cellulitis, or organ failure. |
The majority of patients with Stage 1 or Stage 2 bedsores can recover within a period of 2-3 weeks when prompt treatment is applied. However, the prognosis worsens for those with Stage 3 or 4 bedsores. Of those with Stage 4 bedsores, mortality rates can climb up to 70% within 180 days of onset.
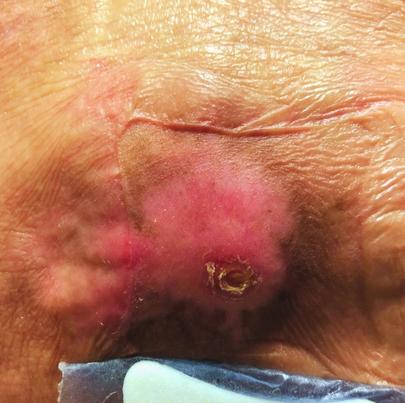
Stage 1 Bedsores - These bedsores are typically mild and will appear as either light or dark red depending on the individual's skin tone. They are identified because the skin surrounding the sore won't blanch when it is pressed. These sores typically feel warm and will cause pain when touched. Stage 1 bedsores can develop quickly, sometimes as short as a few hours.
Stage 2 Bedsores - Stage 2 bedsores manifest as open wounds. These often appear as craters that are often surrounded by fat deposits around their edges. Often, these sores are similar in appearance to blisters and may have a pinkish hue.
Stage 3 Bedsores - These are deep wounds that can reach far into tissue. They are often accompanied by dead, yellowish tissue around the edge of the sore. These sores are often infected and will not heal without the application of medical treatment, including antibiotics.
Stage 4 Bedsores - Stage 1-3 bedsores that are not treated can quickly become Stage 4 bedsores. These sores extend beyond the skin tissue and may lead to the exposure of bones, muscles, and tendons. These sores typically do not cause physical pain because, by the time the pressure sore has reached this stage, it has killed all healthy tissue and nerve endings in the affected area. Stage 4 bedsore life expectancy is lower, and these deeper sores have a significantly high mortality rate.
Stage 4 Bedsore Life Expectancy
Quick Answer: Stage 4 bedsore life expectancy depends on the resident’s age, overall health, infection status, treatment response, and whether the wound has caused complications such as sepsis, osteomyelitis, cellulitis, or organ failure.
A Stage 4 bedsore is a severe pressure wound that extends beyond the skin and may expose muscle, tendon, or bone. These wounds can be difficult to treat and may become life-threatening when a nursing home resident is elderly, medically fragile, malnourished, dehydrated, or already suffering from other serious health conditions.
Because Stage 4 bedsores can lead to dangerous infections, life expectancy can vary significantly from one resident to another. Some residents may improve with aggressive wound care, antibiotics, pressure relief, nutrition support, and close medical monitoring. Others may experience rapid decline if infection spreads or if the wound is not treated promptly.
Factors that may affect Stage 4 bedsore life expectancy include:
- Sepsis: A severe infection that spreads through the bloodstream and can cause organ failure.
- Osteomyelitis: A serious bone infection that may develop when a deep pressure sore reaches the bone.
- Delayed wound care: The longer a Stage 4 bedsore goes untreated, the greater the risk of infection and further tissue damage.
- Malnutrition or dehydration: Poor nutrition and hydration can make it harder for the body to heal.
- Immobility: Residents who are not repositioned regularly may continue to experience pressure on the wound.
- Underlying medical conditions: Diabetes, vascular disease, immune system problems, and other conditions can worsen the prognosis.
When a Stage 4 bedsore develops in a nursing home, families should ask when the wound was first discovered, how often the resident was repositioned, whether a wound care specialist was consulted, and whether the facility followed the resident’s care plan.
Bedsore Life Expectancy and Related Illnesses
Bedsores often cause infections such as sepsis that can quickly spread throughout the bloodstream. They can also lead to the development of squamous cell carcinoma, cellulitis, and meningitis. These conditions can complicate the treatment of existing medical issues, seriously affect the resident’s quality of life, and become life-threatening. When preventable pressure sores cause serious harm, they may support a personal injury claim or nursing home neglect claim.
When Can Bedsores Be a Sign of Nursing Home Neglect?
Quick Answer: Bedsores may be a sign of nursing home neglect when staff fail to reposition immobile residents, monitor skin changes, keep residents clean and dry, provide proper nutrition and hydration, or seek timely medical treatment after a pressure sore appears.
Not every bedsore is automatically caused by neglect. Some residents have serious medical conditions that make pressure sores more likely. However, advanced, untreated, infected, or worsening bedsores may suggest that a nursing home failed to provide proper care.
Nursing homes are expected to monitor residents who are at risk for pressure sores and take reasonable steps to prevent them. This may include repositioning residents, checking skin condition, changing bedding and clothing, keeping residents clean and dry, providing enough nutrition and hydration, and obtaining medical treatment when a wound appears.
Possible warning signs of nursing home neglect include:
- Staff cannot explain when the bedsore first appeared.
- The wound was not documented in the resident’s chart.
- The resident was left in the same position for long periods of time.
- The resident’s clothing, bedding, or skin was frequently wet or soiled.
- The nursing home delayed calling a doctor or wound care specialist.
- The bedsore worsened from Stage 1 or Stage 2 to Stage 3 or Stage 4.
- The resident developed infection, fever, confusion, drainage, odor, or sudden decline.
If a loved one developed serious or worsening pressure sores in a nursing facility, an Illinois nursing home neglect lawyer can help review medical records, photographs, care plans, wound documentation, and staffing issues to determine whether neglect may have contributed to the injury.
Liability for Bedsores

Nursing home providers may be responsible when neglect occurs within their facility. Staff, managers, and owners can potentially be held liable for personal injuries, medical expenses, pain and suffering, and the impact that pressure sores have on a resident’s quality of life. They may also be held liable if an untreated bedsore leads to serious infection, hospitalization, or the untimely death of the resident. A Chicago nursing home neglect lawyer can help gather documentation, including photographs, witness statements, care plans, wound records, and medical records that show how the bedsore developed and progressed.
What Should Families Do If They Discover a Bedsore?
Quick Answer: If you discover a bedsore on a nursing home resident, ask when it was first documented, request the care plan and wound care records, take photos if possible, ask whether a doctor or wound specialist has evaluated the wound, and seek legal guidance if the sore worsened because of delayed care.
Families are often the first to notice changes in a nursing home resident’s condition. If you see a bedsore, bandage, foul odor, drainage, fever, confusion, or a sudden decline in health, it is important to ask questions and document what you observe.
Steps families can take include:
- Ask when the bedsore was first discovered: The nursing home should be able to explain when the wound appeared and how it was documented.
- Request the resident’s care plan: The care plan may show whether the facility identified the resident as being at risk for pressure sores.
- Ask for wound care records: These records may show whether the wound was measured, photographed, cleaned, dressed, and monitored.
- Take dated photographs: If appropriate and permitted, photos can help document the wound’s appearance and progression.
- Ask whether a doctor or wound specialist has evaluated the sore: Advanced bedsores often require prompt medical attention.
- Watch for signs of infection: Drainage, odor, fever, swelling, redness, confusion, or weakness may indicate a serious medical problem.
- Seek outside medical care if necessary: If the resident appears seriously ill, families should not rely only on the nursing home’s assurances.
- Contact a nursing home neglect attorney: If the wound was ignored, untreated, or allowed to worsen, legal action may be appropriate.
Families should also keep notes of conversations with nursing home staff, including names, dates, explanations given, and any changes in the resident’s condition. These details may become important if the bedsore leads to hospitalization, infection, or a potential neglect claim.
What to Look For
When visiting a relative at the nursing home, loved ones should be sure to ask the attending staff to show them the areas of the body where bedsores are mostly found. Visitors can also pay attention to any foul odors when entering the room. Bedsores will often emit an odor.
It is also a good idea to look for any bandages or dressing in the lower back and buttocks area. If they are present, it could mean the presence of a bedsore.
If a relative is unexpectedly on a regimen of antibiotics, family members might also ask if the medication is for an active infection and if it stems from a bedsore.
Bedsore Life Expectancy FAQs
What is the life expectancy of someone with bedsores?
Bedsore life expectancy depends on the stage of the wound, the resident’s overall health, how quickly treatment begins, and whether complications develop. Early-stage bedsores may heal with prompt care, while Stage 3 and Stage 4 bedsores can become life-threatening if infection spreads.
How serious is a Stage 4 bedsore?
A Stage 4 bedsore is a severe pressure wound that may expose muscle, tendon, or bone. These wounds can lead to serious infections, sepsis, hospitalization, surgery, and in some cases death, especially among elderly or medically fragile nursing home residents.
Can bedsores cause death?
Yes. Bedsores can cause death when they lead to severe complications such as sepsis, cellulitis, bone infection, meningitis, or organ failure. The risk is higher when pressure sores are advanced, infected, untreated, or allowed to worsen over time.
Are bedsores a sign of nursing home neglect?
Bedsores may be a sign of nursing home neglect when staff fail to reposition residents, monitor skin condition, keep residents clean and dry, provide proper nutrition and hydration, or obtain timely medical treatment. Not every bedsore is caused by neglect, but advanced or worsening wounds should be investigated.
What infections can bedsores cause?
Bedsores can lead to infections such as cellulitis, sepsis, osteomyelitis, and meningitis. These infections can spread quickly and may become life-threatening if the resident does not receive proper medical care.
What should families do if a nursing home resident has bedsores?
Families should ask when the bedsore was first documented, request the care plan and wound care records, take photographs if possible, ask whether a doctor or wound specialist has evaluated the wound, and seek outside medical care if the resident appears seriously ill. If the wound worsened because of delayed care, contacting a nursing home neglect lawyer may be appropriate.
Call: (312) 609-0400
or fill out the Contact Form

.svg)
 Motor Vehicle Accidents
Motor Vehicle Accidents 



